Guest Blogger Letter:
Dear Mr. Sparks,
Could you take a moment and read my daughter’s story? I know
your books are a fantasy, but this is reality for all of us affected by CDH.
The reality is there even when people don’t want to face
it. The reality is my daughter didn’t
get the perfect beginning. She didn’t
get to cry and be placed in her mom’s arms (or dad’s arms) for comfort. When
she cried, she was whisked away to a different operating room to be
intubated. People don’t want to face the
reality of it all. I have had several
family members tell me they didn’t want pictures of her with all those tubes. Those tubes were our reality. Why shouldn’t we have pictures up with her
tubes? Why should we pretend it never happened? The reality is my daughter was
born with Congenital Diaphragmatic Hernia.
The reality is my daughter was very sick when she was born. The reality is my daughter survived.
Ryan and I found out that we were pregnant on Thanksgiving
Day 2012. I didn’t take the pregnancy
test until the very end of the day because I didn’t want to be heartbroken when
the test came back negative. We were overjoyed to be expecting our first
child. I knew immediately we were having
a little girl. Call it mother’s intuition.
I felt sick all the time.
I wasn’t able to eat anything besides pasta and cheese pizza. Around 17
weeks I ate a cheeseburger without feeling sick for the first time and was so
excited to feel normal.
At 19 weeks we had our gender and anatomy scan. My mom and Ryan’s mom came with us. When the tech told us the baby was a girl I
yelled, “I knew it!” We really didn’t care either way, I just hate being
wrong. After the doctor looked at the
ultrasound, we were asked to meet with him for a minute. Our moms waited in the waiting room for us
and we met with the doctor. He told us
our daughter had fluid around her lungs, this was called pleural effusion. This could mean a number of things anything
from a chromosomal disorder like Down’s syndrome or it could be nothing. He wanted to see us again in a week to
evaluate the amount of fluid and to see if there were any changes. Ryan and I were scared. We didn’t tell any of
our family and actually lied saying the reason we were having more ultrasounds
was due to me just being diagnosed with hypothyroidism a month prior to
becoming pregnant. We didn’t want to worry anyone until we knew what we were
dealing with.
At 20 weeks the ultrasound looked about the same and we were
told to come back in two weeks to see if there was any change. After our 22 week ultrasound we were being
referred to the St. Louis Fetal Care Institute (FCI) at Cardinal Glennon. Our
doctor didn’t have the technology to assist us anymore.
The first day at Fetal Care Institute was long and
overwhelming. We had an entire day scheduled out for us that included meeting
everyone from our social worker to our doctor.
We had our first 3D/4D ultrasound of our daughter, Lucie. We could see
Lucie’s features and could tell she looked like me. As I lay in the chair for
our ultrasound, we met our doctor, Dr. Vlastos. Dr. Vlastos had a way about him
that we fell in love with immediately.
After introducing himself, he told us, “Let’s take a look at the babe.”
He pointed out all Lucie’s anatomy and pointed out that there was “something in
Lucie’s chest.” He went onto explain that he believed her intestines were in
her chest. Lucie had congenital
diaphragmatic hernia.
Up until this point, Ryan and I didn’t have any idea what
was wrong. It could be any number of
things. To hear a diagnosis was actually a comfort. Even if it was the beginning of more fear, we
were comforted to know what was wrong.
Then the fear kicked in.
I went home and did a little research to understand the
diagnosis better. I found a website for
an organization called CHERUBS. The only
other place I was finding anything helpful was from the DRHEAMS research study. I learned that these babies only have 50%
survival rates.
At 25 weeks I went back to FCI for an MRI to confirm Dr.
Vlastos diagnosis. Lucie had left-sided
CDH (the hole in her diaphragm was on the left side) and her intestines were in
her chest pressing against her left lung.
Her heart was slightly pushed to the right side. Lucie had a predicted
lung volume of 40% so they felt that she had a fighting chance. One thing I
learned very quickly was that even if your CDHer had a good prognosis, it
didn’t mean anything. Some babies who
had the worst prognosis survived with others with great chances did not. Dr.
Vlastos told me that Lucie had a good chance, but she was safest in the womb.
The following week we went for another check up with Dr.
Vlastos. We met with a neonatologist and
her surgeon, Dr. Chatoorgoon. I was able to hear what the surgeon had to say
with very little fear. He told us that Lucie would have her repair as soon as
she was stable enough to survive surgery. They would push her intestines back
into the abdomen and repair the hole. After that, she would remain in the
hospital as long as it was necessary for her lungs to develop and survive.
It was talking with
the neonatologist and hearing what would happen when she was born that sent me
over the edge. I could barely hear the
words without tears streaming down my face.
Ryan held my hand as I cried. Lucie would be born vaginally if
possible. As soon as she was born she
would be taken to be intubated. After
being intubated, Ryan and I would have the opportunity to see her. If we choose to, the rest of our family could
see her briefly. She then would be
transferred to Cardinal Glennon. We would not have the opportunity to hold her.
I dealt with lots of emotions through the next few
months. I considered changing Lucie’s
name in case she didn’t make it. I had
picked out the name Lucie when I was 10 and didn’t want my Lucie not to
survive. I contemplated not having any
baby showers, but ended up having 6 different ones. I told everyone that I had
no doubt that she would survive. Every
day I feared that she wouldn’t live. I
feared that I would never hold my child alive.
We toured the high risk hospital that we would deliver at. I
am pretty sure we made the others touring with us uncomfortable and probably
fearful. We asked questions about babies
being intubated, babies being transferred to the Cardinal Glennon, would we be
able to see the baby before they are transferred, and other questions expecting
parents don’t want to think about. Maybe I should have asked these questions
privately, but I was afraid I wouldn’t have the opportunity to ask later.
I was finishing up my school year and going to see FCI every
2 weeks. Lucie was thriving. The fluid around her lungs was still there, and
there was still no explanation for it being there. Lucie was also developing hydrops (swelling
under the skin), and I had developed polyhydramnios (excess amniotic fluid). At 34 weeks I had 41 cm of amniotic fluid when
someone at 34 weeks should roughly have only 21 cm of fluid. It was becoming more difficult to breath and
much more uncomfortable.
At 32 weeks, Lucie’s pleural effusion and hydrops was
looking worse and I was admitted to St. Mary’s Medical Center until further
notice. Dr. Vlastos was out of town and the other doctor told us to go home,
pack a bag and then head to the hospital.
They would call ahead to the hospital so they would be prepared for us. Traffic
was horrible so we decided to go straight to the hospital and have my
mother-in-law take care of my bag. We decided to have one last meal together
before I was admitted to the hospital.
There was a sandwich and cheesecake shop across the street from the
hospital. The place was called Daddy’s
and it felt fitting that we should eat there.
When we got to the hospital we were told they had no idea we
were coming. No one was sure what they were supposed to do with us. Eventually, the hospital staff figured out
who we were and settled me into a room. I was put on continuous monitoring.
Being on continuous monitoring was so uncomfortable. I couldn’t move much or the monitor wouldn’t
pick up Lucie. My sciatic nerve would
shoot pain through my back and legs because Lucie was pushing on it and I
couldn’t move out of that position. I
was extremely tired, but sleep didn’t come easy. I could have my child at any time, but ideally
we had to keep her put for another couple weeks. We didn’t want her to come prior to 38 weeks
if possible. After 5 days in the
hospital, I was told that the monitoring Lucie had been very reactive during
all the monitoring and I could go home and do the same thing I was doing in the
hospital.
I eagerly went home, had my last 2 baby showers, and relaxed
as I much as I could. Twice a week I
went to FCI to have a non stress test and ultrasound. I was getting pretty good at reading the
ultrasounds and enjoyed guessing what things were with the ultrasound tech,
Cindy. Lucie was staying stable.
At 35 weeks, she was even more swollen and to keep her in me
for as long as possible I was readmitted to the hospital indefinitely. We had an EXIT procedure (a special type of
c-section that gives the baby a better chance of survival outside of the womb)
scheduled for 37 weeks. I was very nervous and sad to have an EXIT procedure
because I would be under anesthesia and Ryan would not be able to be in the
operating room with me. I had a great fear that Lucie wouldn’t survive long
enough for me to wake up from the anesthesia.
For 4 days, I was on continuous monitoring. Once an hour I
was able to get up to use the restroom and that was it. I was even bigger
because the fluid kept increasing and Lucie was getting bigger.
I finally was given the okay to be moved to a different room
and be on intermittent monitoring. I was able to move around my room and once a
day Ryan was able to take me on a wheelchair ride. We visited the chapel and prayed or we would
go outside and sit next to a waterfall in front of the hospital.
A week before our planned EXIT procedure, I was given the
best news. Lucie seemed to be doing so
well and things weren’t getting worse that we could have a traditional
c-section. We were so excited that Ryan could be with me in the operating
room. We now had a new plan.
June 30th I couldn’t sleep. I was uncomfortable, I had to pee every half
hour, and I was nervous. The transport
nurse Mary came to pick me up at 4:30 a.m. She told me that she was the only
person there only for me. Everything I
needed, she would take care. I was
wheeled to the ambulance and Ryan drove to Cardinal Glennon separately. I will
never forget the feeling of my belly swaying back and forth with every turn in
the ambulance.
I was ushered in through the ER and wheeled to FCI. I was ushered into the ultrasound room to be
prepared for surgery and for one last peek at Lucie. My family joined me for
hugs before the big moment. And then it was time.
Ryan walked with me and waited outside of the OR while I
received my epidural. The nurses from FCI and Mary held me while I received my
epidural. I was laid down and Ryan was
finally able to join me in the OR. Ryan held my hand the entire time.
Before Lucie was delivered, the fluid from around her lungs
need to be removed. Dr. Vlastos used a needle to remove some of the fluid, but
not all of the fluid was removed. It’s
funny looking back at what I remember from the c-section because I really don’t
remember most of it. One thing I do remember was when they broke my water I
heard it splash and saw it come over the curtain. I was later told that I had 2 gallons of
amniotic fluid.
The moment Lucie let out a cry, I couldn’t have been happier
in my entire life. The moment she let out her second cry, I lost it. Ryan was
standing next to me holding my hand and watching Lucie be born. Immediately,
Lucie was rushed out of my OR room to her OR room to be intubated. It felt like
ages before Ryan was given the okay to go see her. In reality, it was only about 15 minutes.
Dr. Chatoorgoon took Ryan over to see her. He was able to
hold her hand and take pictures to show me.
The first time I saw what Lucie looked like was in a picture. She was big. She weighed seven pounds
fourteen ounces. After a little bit the
surgery team brought Lucie over for me to see. I held her hand and cried. I told her I loved her. And as quickly as she
came in, she was taken away again.
After I recovered, I was brought up to the NICU on a
stretcher. I don’t remember much of the
half hour I spent with her. She was
doing really well and her NICU room was crowded with Ryan and me and our family
taking turns coming in to visit with me and Lucie. Many pictures were
taken. Looking back on it, it was
probably way too over stimulating for her. I didn’t want to leave her, but I
knew the EMTs actually had other places to be and couldn’t stay all day in the
NICU with me.
Going back to the high risk hospital was one of the toughest
things I ever did. The other toughest
thing I did was go home without my baby.
The first day I pumped every 3 hours and slept. Ryan spent
the entire day with Lucie and came to the hospital to be with me that
night. He helped me sit up to pump,
clean my pumping tubing, and do anything I needed that I couldn’t do stuck in
bed.
That night I was awakened by my phone ringing. I tried to wake Ryan, but he was exhausted
from the day and I don’t think I really tried very hard. It was the NICU calling to give me an update. Now a call from the NICU in the middle of the
night is not a good update- ever. What makes it worse is when you are on
morphine and really have no idea what they are talking about. I had no idea what a good O2 level was and
what a bad CO2 level was. I hadn’t spent
the day in the NICU. I had spent the day
in my hospital bed, away from my child, recovering from major surgery, and
praying that I would be able to spend time at the NICU the next day.
When Lucie was born, she was put onto a traditional
ventilator. At her 10:00 blood gas, he CO2 levels were high meaning her body wasn’t
pushing the CO2 out of the blood stream, so they switched her to an oscillator which
gave her lungs an opportunity to expand. I was also told things weren’t looking
good. Chances were she would be on ECMO
by morning. ECMO is a heart and lung bypass machine which would give her heart
and lungs the time to heal without being used to sustain her life. To me ECMO
was what I wanted to avoid at all costs.
I called in the morning to check on her, and she was doing
much better. Her CO2 levels had come
down and she was stable. I wasn’t able to go visit her until the afternoon.
When I was wheeled into her room it was a completely different feel than the
day before. The room lights were dimmed
as low as they could be and still be on.
The oscillator was extremely loud.
Her entire body moved with every breatht he machine took for her and
since it had her breathing 600 times per minute, she was shaking constantly. Lucie
had her bonding baby covering her eyes and ear muffs covering her ears. I was
completely overwhelmed. I was scared to
touch her at all, but I longed to hold her hand more than anything. I sang to her, I read to her, and I stared at
her while she lay there sedated.
On July 3 they switched Lucie back to a traditional
ventilator to see how she would do. When we left for the evening she wasn’t
releasing the CO2 as well as they wanted and we were warned that she may be put
back on the oscillator in the middle of the night. After her 10:00 blood gas
she was put back on the oscillator.
After four more days on the oscillator she was put back on
the traditional ventilator and did well on it.
Her oxygen levels were in the 90s, which was excellent. At 9 days old I
was able to hold Lucie. It was quite a
production because of all of the tubes. I never wanted to let go of her, but I
barely was able to hold her.
 She had her repair at 10 days old. Remember how I said that
leaving her at the hospital and going home were 2 of the worst days of my life,
well her surgery day tops that list as well. We went into the hospital early so
we can have some time with her before the surgery team came to prep her for
surgery. We talked with her and prayed with her. Judy from pastoral care came to pray over
Lucie with us. Judy will forever be special to us.
She had her repair at 10 days old. Remember how I said that
leaving her at the hospital and going home were 2 of the worst days of my life,
well her surgery day tops that list as well. We went into the hospital early so
we can have some time with her before the surgery team came to prep her for
surgery. We talked with her and prayed with her. Judy from pastoral care came to pray over
Lucie with us. Judy will forever be special to us.
The surgery team came in to prepare her for surgery around
7:00 a.m. They had to disconnect her from the ventilator and manually bag her
to keep her breathing while the transferred her to the operating room. Everything that was sustaining her life had
to be brought with her to the operating room.
When Lucie was wheeled out of the room Ryan just held me as
I cried. The room that had been filled
with machines and our daughter was now empty. I had to wait and trust in a team
of people I barely knew to save my daughter’s life. We waited 4 and half hours
for Lucie’s surgery to be finished.
Lucie’s hole was
larger than the surgeon had anticipated.
He tried to repair it without a gortex patch, but the repair started to
rip before he had finished sewing it together. He used the gortex patch to
repair the hole. Our surgeon felt very
confident that everything went excellently.
The night of her surgery I stayed at the hospital with her.
She was on fentynal for the pain, but she was experiencing more pain than
normal. It broke my heart because you could see the pain in her eyes. I’m so
glad that I stayed that night because her nurse wasn’t as familiar with Lucie
and didn’t know Lucie’s normal heart rate and blood pressure. I was able to tell her that Lucie’s heart
rate was high and she was in pain.
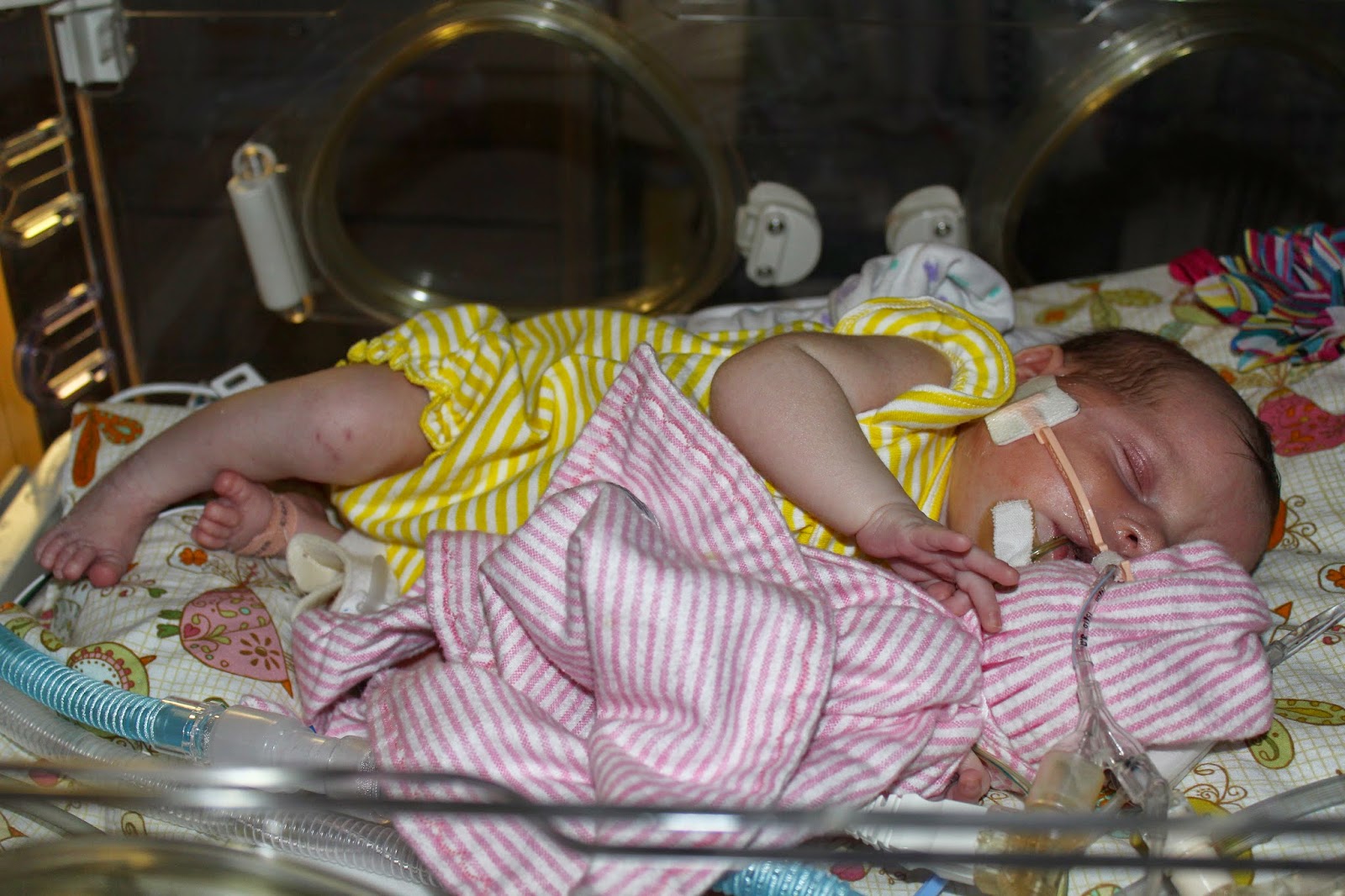 It only took 9 more days for Lucie to begin breathing
completely on her own. During that time
she continued to heal and began to become more awake and active. She was
extubated at 19 days old. She tried over and over to extubate herself before
the doctor came in to do it. Once she was taken off the ventilator, she was put
on a high flow nose cannula. It blew forced air into her nose to ensure that
she was getting enough oxygen.
It only took 9 more days for Lucie to begin breathing
completely on her own. During that time
she continued to heal and began to become more awake and active. She was
extubated at 19 days old. She tried over and over to extubate herself before
the doctor came in to do it. Once she was taken off the ventilator, she was put
on a high flow nose cannula. It blew forced air into her nose to ensure that
she was getting enough oxygen.
Her weak little cry
was the most beautiful thing I ever had heard.
Ryan came by the hospital on his lunch break just to see her without a
tube down her throat. We were overjoyed.
Now all we had to do was get her off the nose cannula and get her
eating. Lucie was stronger than ever at this point and was off the nose cannula
in a few short days.
 Lucie went home July 29 without any respiratory support or
feeding support. I was thrilled. She has
been fortunate enough to not have any issues that have landed her back in the
hospital since we brought her home.
Lucie went home July 29 without any respiratory support or
feeding support. I was thrilled. She has
been fortunate enough to not have any issues that have landed her back in the
hospital since we brought her home.
Our reality is very different than other CDH families. Our
reality may not be the perfect beginning.
Our reality may have been very different than what I envisioned when I
dreamed about becoming a mom, but our reality is a dream come true. Our reality
is that our daughter survived.
Mr. Sparks, thank you for reading my daughter’s story. I hope she inspires you write about this
reality that we have all faced. Some of
our realities end with a child coming home healthy and happy. Others have their reality end bringing their
child home on much needed medical support and happy. Others have their reality end by not bringing
their child home. This is a reality I
pray that can be stopped. The only way
to stop it is for more funding for research.
The only way for more funding for research is for more awareness. Please, Mr. Sparks, consider writing about a
CDH family in one of your upcoming novels. These are love stories like none
other.
Sincerely,
Laura Henderson
Mom to left sided CDHer Lucie born 7/2013



I'm very happy to read about how well your daughter did, after the repair! I think others who are carrying a baby with CDH will read your story and find hope and strength from it.
ReplyDeleteMy daughter was born back in 1990, with the same condition. Her repair went well. Her incision was twice as big, but that could have been just how they did it back then. She was in the hospital for four months, but then started getting better, slowly but surely. She's grown, now and not limited by having been born with CDH, at all! Best wishes to you and your daughter, for the future!